Heart Health in the Workplace: A Safety Perspective on Cardiac Preparedness
Posted by Anthony Webb on Feb 12th 2026
Heart Health in the Workplace: A Safety Perspective on Cardiac Preparedness

Cardiac emergencies at work are often seen as medical incidents, but from a safety perspective, they are response events shaped by the conditions of the job. In industrial settings, survival during a sudden cardiac emergency depends less on medical history and more on where the work takes place, who is present, and how prepared the workplace is to respond.
At MCR Safety, we work closely with distributors, employers, and workers across construction, manufacturing, utilities, energy, transportation, and maintenance. To better understand how cardiac emergencies intersect with real-world job conditions, we evaluated guidance from OSHA, the CDC, and cardiovascular safety organizations alongside occupational work-context data from the U.S. Department of Labor’s O*NET program. These sources show that workplace factors like recognition, response time, environmental stress, and preparedness often have a greater impact on cardiac outcomes than individual health profiles.
This article outlines why cardiac emergencies are a workplace safety concern and summarizes recommendations from recognized safety authorities. The goal is to support effective safety planning and reinforce the importance of readiness in the event of medical emergencies at work.
Why Cardiac Emergencies Are a Workplace Safety Issue

Sudden cardiac arrest (SCA) is frequently confused with a heart attack, but the distinction is critical in workplace settings. A heart attack occurs when blood flow to the heart muscle is blocked. Sudden cardiac arrest results from an electrical malfunction that causes the heart to stop beating effectively and requires immediate intervention (1).
According to the Occupational Safety and Health Administration, an estimated 10,000 sudden cardiac arrests occur each year in U.S. workplaces, representing a meaningful share of workplace fatalities (2). The Centers for Disease Control and Prevention further notes that many cardiac events occur outside of hospitals, and survival depends heavily on rapid recognition and response (3).
From a safety standpoint, cardiac emergencies should be treated as credible workplace events and planned for with the same seriousness as fires, chemical releases, or severe injuries.
Where Outcomes Are Most Affected: Delayed Response and Isolation

Across OSHA, CDC, and sudden cardiac arrest awareness materials, one conclusion is consistent: time to response is the most critical factor influencing survival (2)(3)(4).
To better understand response limitations, we reviewed occupational work-context data across industrial roles where emergency access is frequently delayed. O*NET data shows that occupations such as utility line workers, field service technicians, energy-sector maintenance workers, and remote equipment operators consistently score in the upper-80s to 90s range for independent work, small crew environments, and distance from centralized support.
These conditions do not make cardiac events more likely, but they do increase the impact by delaying recognition, limiting immediate assistance, and extending the time before professional medical care arrives.
In these environments, preparedness is the most controllable factor influencing outcomes, rather than proximity to hospitals.
Physically Demanding Work Amplifies Cardiac Emergencies
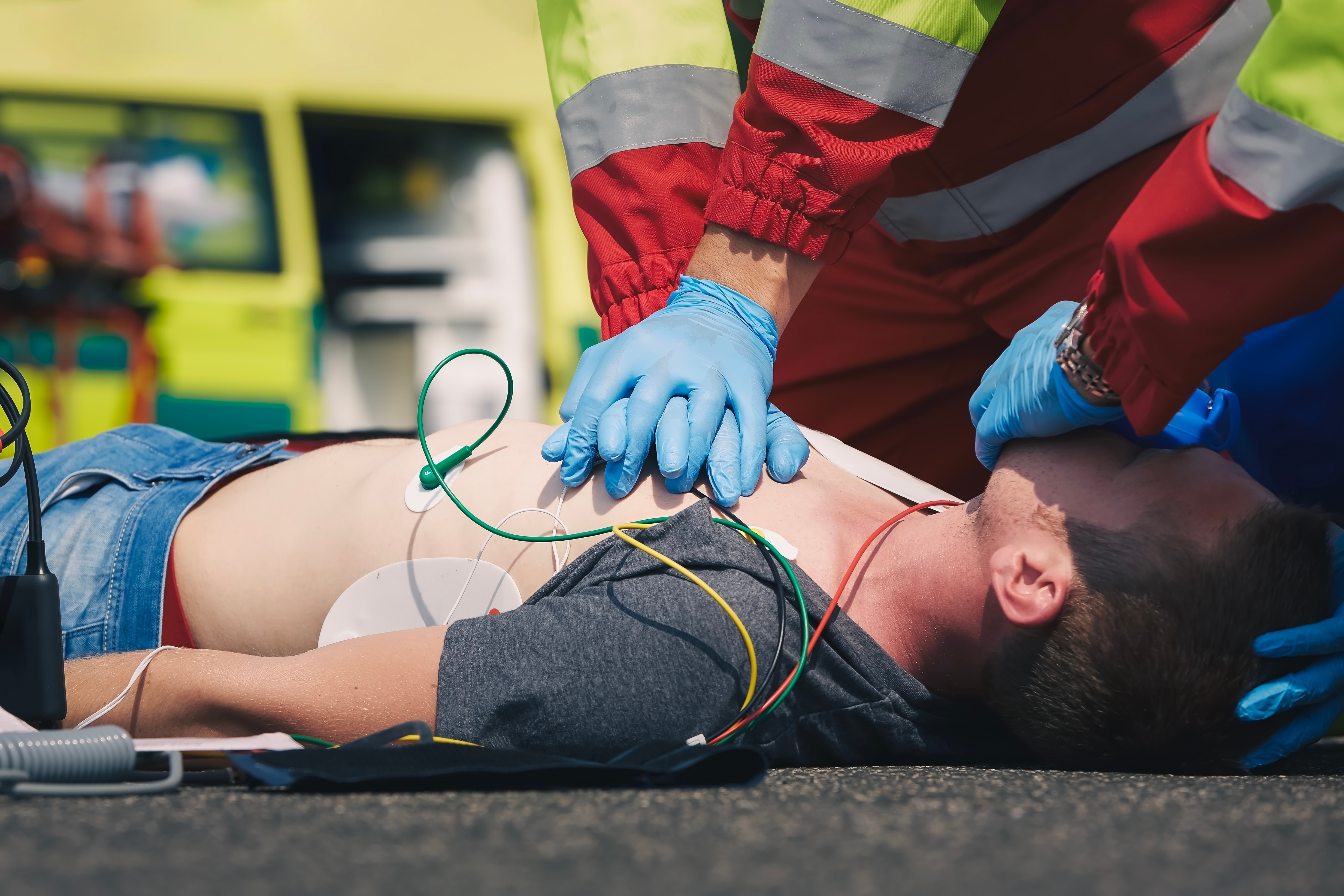
Physical exertion is a defining feature of many industrial jobs. Construction labor, industrial maintenance, utility repair, manufacturing operations, and energy-sector roles frequently require sustained effort, manual handling, climbing, and repetitive motion.
O*NET data shows that occupations such as utility line workers, field service technicians, energy-sector maintenance workers, and remote equipment operators consistently score in the upper-80s to 90s range—on a 0–100 occupational scale—for independent work, small crew environments, and distance from centralized support.
CDC and American Heart Association guidance recognize that physically demanding work increases cardiovascular strain, particularly when combined with other stressors such as heat or fatigue (3)(5). Importantly, occupational exertion is not the same as cardiovascular conditioning. High physical strain can elevate heart rate and blood pressure without offering the protective benefits of structured aerobic activity.
From a safety perspective, the concern is not whether demanding work causes heart disease, but that high exertion lowers tolerance for delayed recognition and response, making cardiac emergencies more severe when they happen.
Environmental Stress Makes Emergencies More Dangerous

Environmental conditions further compound cardiac risk at work. The CDC and OSHA repeatedly identify heat exposure, dehydration, outdoor work, and non-climate-controlled environments as factors that increase physiological stress and complicate emergency response (3)(6).
O*NET environmental-exposure data reinforces this concern. Roles such as utility line workers, oil and gas field workers, roofers, agricultural equipment operators, and outdoor maintenance personnel frequently score in the highest exposure bands—often in the upper-80s or higher—for extreme temperatures and environmental stress.
In these conditions, cardiac emergencies are harder to detect early and become more dangerous when response is delayed. This highlights the need for preparedness plans that reflect how work is performed, not just where it takes place.
Preparedness Is a Core Element of Safety Culture

OSHA guidance is clear that immediate CPR combined with rapid defibrillation can double or even triple survival rates compared to waiting for emergency responders alone (2). Automated external defibrillators (AEDs) are built to guide responders’ step by step and cannot deliver a shock unless the device determines it is necessary, reducing hesitation during emergency response.
Effective workplace preparation includes:
- Emergency response plans that address medical emergencies
- Training to recognize sudden cardiac arrest and activate response protocols
- Awareness of AED locations and assigned response roles
- Clear communication procedures
- Periodic review and reinforcement of emergency protocols
Cardiac preparedness should follow the same framework used for other serious hazards: define responsibilities, reduce response time, and remove uncertainty before an emergency happens.
Safety Means Protecting the Whole Person
Modern workplace safety extends beyond visible hazards alone. OSHA and CDC guidance emphasize that organizations with strong emergency preparedness programs tend to demonstrate more resilient safety cultures overall (2)(3).
Protecting workers means understanding that serious medical emergencies can happen during routine job activities. While cardiac events are medical, survival at work often depends on readiness, coordination, and response before professional care is available.
Protecting People Means Preparing for the Unexpected

Cardiac emergencies are medical events, but workplace conditions and preparedness often shape survival outcomes.
At MCR Safety, we approach protection by evaluating the full work environment, including job demands, exposure conditions, and the protective equipment workers use every day. Preparedness is most effective when hazard assessment, PPE selection, and safety education are integrated, intentional, and aligned with real job conditions.
This is the foundation of our 360° approach to protection and shows why preparation, awareness, and PPE are most effective when they work together.
We Protect People.

Learn more about MCR Safety by checking out our most recent video. For more information, browse our website, find a distributor, or give us a call at 800-955-6887.

